-
About
Our Story
back- Our Mission
- Our Leadershio
- Accessibility
- Careers
- Diversity, Equity, Inclusion
- Learning Science
- Sustainability
Our Solutions
back
-
Community
Community
back- Newsroom
- Webinars on Demand
- Digital Community
- The Institute at Macmillan Learning
- English Community
- Psychology Community
- History Community
- Communication Community
- College Success Community
- Economics Community
- Institutional Solutions Community
- Nutrition Community
- Lab Solutions Community
- STEM Community
- Newsroom
- Webinars on Demand
- Digital Community
- The Institute at Macmillan Learning
- English Community
- Psychology Community
- History Community
- Communication Community
- College Success Community
- Economics Community
- Institutional Solutions Community
- Nutrition Community
- Lab Solutions Community
- STEM Community
- Newsroom
- Webinars on Demand
- Digital Community
- The Institute at Macmillan Learning
- English Community
- Psychology Community
- History Community
- Communication Community
- College Success Community
- Economics Community
- Institutional Solutions Community
- Nutrition Community
- Lab Solutions Community
- STEM Community
- Newsroom
- Webinars on Demand
- Digital Community
- The Institute at Macmillan Learning
- English Community
- Psychology Community
- History Community
- Communication Community
- College Success Community
- Economics Community
- Institutional Solutions Community
- Nutrition Community
- Lab Solutions Community
- STEM Community
- Newsroom
- Macmillan Community
- :
- Psychology Community
- :
- Talk Psych Blog
- :
- Why Do Americans Spend Much More on Health Care, Y...
Why Do Americans Spend Much More on Health Care, Yet Die Sooner?
- Subscribe to RSS Feed
- Mark as New
- Mark as Read
- Bookmark
- Subscribe
- Printer Friendly Page
- Report Inappropriate Content
The history of Americans' health is, first, a good news story. Thanks to antibiotics, vaccines, better nutrition, and diminished infant mortality, life expectancy-at-birth has doubled since 1880—from 38 to 79 years. For such a thin slice of human history, that is a stunning achievement. Even amid a pandemic, be glad you are alive today.
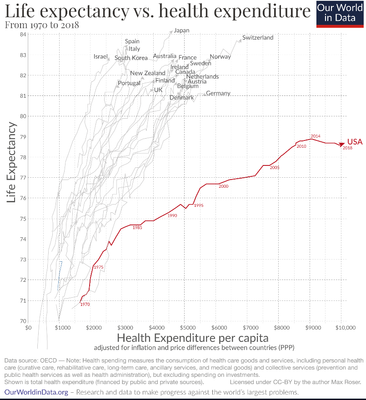
The recent not-good news is that, despite doubled per-person health-care spending compared to other rich countries, U.S. life expectancy is lower—and has been declining since 2014.
Can you guess why Americans, despite spending more on their health, are dying sooner?
Our World in Data founder, Max Roser, sees multiple explanations.
- Smoking. While the COVID-19 pandemic has claimed 2.4 million lives in the past year, cigarette smoking kills 8.1 million people annually—and it kills more in the U.S. than in other wealthy countries. Of those people who are still smokers when they die, two-thirds die because of their smoking. Still, there’s some good news: The plunging smoking rate is reducing both smoking-caused deaths and the smoking fatality gap between the U.S. and other rich countries.
- Obesity. While smoking has declined, obesity—a risk factor for heart disease, stroke, diabetes, and some cancers—has increased: 36 percent of Americans are now obese. Compared to the other rich (but less obese) nations, the U.S. has a much higher rate of premature deaths attributed to obesity (five times that of Japan, more than double that of France, and nearly 60 percent greater than Canada).
- Homicides. As a gun-owning culture, Americans much more often kill each other—four times more often than the next most murderous rich nation (peaceful Canada).
- Opioid overdoses. Like homicides, America’s much greater opioid overdose death rate, though causing less than 2 percent of all deaths, affects life expectancy because so many victims are young.
- Road accidents. A surprise to me—and you?—is the U.S. having, compared to other rich nations, a roughly doubled rate of vehicle-related accidents (again, often involving the young, and thus contributing to the life expectancy gap).
- Inequality and poverty. Although the U.S. enjoys higher average income than most other rich countries, its lower-income citizens are poorer. This greater inequality and poverty predicts less access to health care and also greater infant mortality, which, among the rich nations, is highest in the U.S.
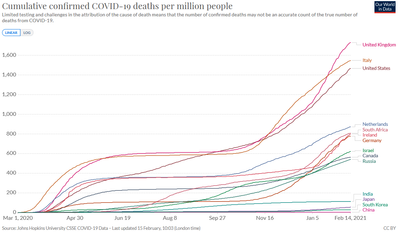
And how might we expect the pandemic to affect the U.S. life expectancy standing? The half-million U.S. COVID-19 deaths in the pandemic’s first year have, per capita, been matched by the UK and Italy, but are roughly double those of other European nations, and many times more than collectivist East Asian countries.
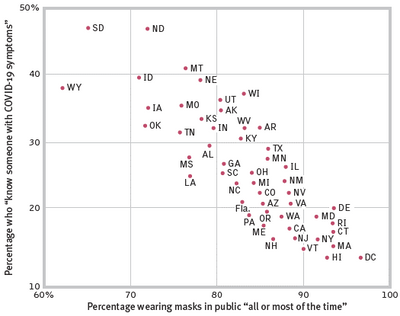
For its often mask-defying rugged individualism, the U.S. has paid a heavy price. Moreover, as Nathan DeWall and I report in our forthcoming Exploring Psychology, 12th Edition (with data from Carnegie Mellon University), there has been a striking -.85 correlation across states between mask wearing and COVID-19 symptoms. Less mask wearing—as in the mask-resisting Dakotas, Wyoming, Idaho, and the Southern states—predicts more COVID-19. The Centers for Disease Control observed the same correlation across U.S. counties during 2020: COVID-19 cases and deaths increased in U.S. counties that reinstated in-person dining or not requiring masks.
As Max Roser notes, the factors that predict Americans’ dying sooner—smoking, obesity, violence, opioids, poverty, and likely COVID-19—are less about better healthcare for the sick than about averting health problems in the first place. As Benjamin Franklin anticipated, “An ounce of prevention is worth a pound of cure.”
(For David Myers’ other essays on psychological science and everyday life, visit TalkPsych.com; follow him on Twitter: @DavidGMyers.)
-
Abnormal Psychology
6 -
Achievement
2 -
Affiliation
1 -
Behavior Genetics
1 -
Cognition
7 -
Consciousness
8 -
Current Events
29 -
Development Psychology
14 -
Developmental Psychology
9 -
Drugs
1 -
Emotion
13 -
Gender
1 -
Gender and Sexuality
1 -
Genetics
3 -
History and System of Psychology
3 -
Industrial and Organizational Psychology
2 -
Intelligence
4 -
Learning
3 -
Memory
2 -
Motivation
3 -
Motivation: Hunger
2 -
Nature-Nurture
4 -
Neuroscience
6 -
Personality
10 -
Psychological Disorders and Their Treatment
10 -
Research Methods and Statistics
22 -
Sensation and Perception
10 -
Social Psychology
87 -
Stress and Health
8 -
Teaching and Learning Best Practices
7 -
Thinking and Language
14 -
Virtual Learning
2
- « Previous
- Next »